What is it?
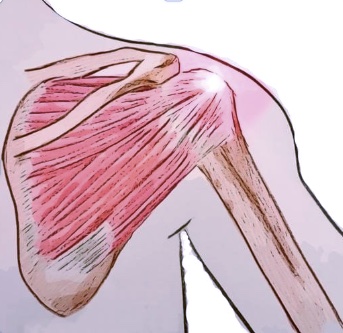
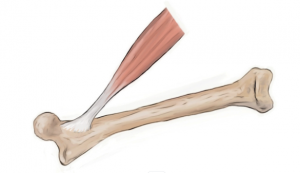
A ring of flexible, fibrous connective tissue, known as the glenohumeral labrum, surrounds the shoulder joint. This labrum increases the stability of the shoulder while allowing for the required flexibility of one of the bodies’ most sophisticated joints. One well-known muscle of the arm, the biceps, has an attachment directly into the labrum and is a common site of injury. A tear of the labrum can occur in many locations, however the most common is at the point where the biceps tendon attaches to the labrum. Usually, this tear follows a typical pattern and is referred to as a superior labrum tear, anterior to posterior (SLAP tear).
What causes it?
SLAP tears can be caused by trauma such as a fall onto an outstretched hand or a dislocated shoulder. Tears can also develop over time with repeated throwing actions or overhead activities as the labrum is weakened and eventually injured. Traumatic tears are more likely to be symptomatic than tears that develop slowly.
What are the symptoms?
As mentioned, SLAP tears can occur suddenly, through trauma or develop slowly through repeated stress. Often if the injury develops over time, patients can be unaware they have sustained a tear and the injury doesn’t have a significant impact on their pain or function. Preexisting SLAP tears can however, place more tension on the long head of biceps tendon, leading to overuse disorders as a secondary complication.
When the tear occurs through a sudden action or trauma, symptoms can be more marked. Sufferers often notice pain deep in the shoulder joint with overhead shoulder movements, a feeling of weakness, loss of power and/or accuracy with throwing activities. Some people may notice a popping or clicking sensation and occasionally the shoulder may give way. In severe tears, the shoulder might feel unstable and even be at increased risk of dislocation.
How can physiotherapy help?
Your physiotherapist is able to help diagnose a suspected SLAP tear and send you for further imaging if needed. SLAP tears are often graded by severity from I to IV as a way to guide treatment. Physiotherapy is usually recommended as a trial for all tears before considering surgical repair and in many cases can effectively help patients return to their previous activities, symptom-free.
If physiotherapy is unsuccessful, surgical repair with a full rehabilitation program is recommended. Surgery will usually either repair the tear or reattach the biceps tendon to the humerus (tenodesis). Following surgery, a period of rest in a sling is required before rehabilitation can begin.
None of the information in this article is a replacement for proper medical advice. Always see a medical professional for advice on your individual injury.